Are migraines and tinnitus related? Ringing in the ears, commonly known as tinnitus, can be associated with several kinds of disorders, including migraine. Vestibular migraine is a common kind of migraine associated with tinnitus, but there are other kinds of migraine-related attacks associated with tinnitus.
Can Migraines affect your ears? Migraine doesn’t cause hearing loss, but some types are associated with tinnitus and other ear problems. It’s fairly well-known that a migraine attack can include changes to vision, such as visual aura, but many people aren’t as aware of the hearing problems and ear-related complaints that can go with the disease.
Why do I keep getting headaches and ringing in my ears? Headache is a common symptom that can result from infection such as meningitis, concussions, or head injuries, exposure to loud noises, or vision problems as well as other conditions. Ringing in the ears can be a result of loud noise exposure or can be related to conditions involving the ears themselves.
What does a tinnitus headache feel like? Tinnitus can be described as an internal head noise that may sound like ringing, buzzing, whooshing, beeping, chirping, or other sounds.
Are migraines and tinnitus related? – Additional Questions
Does tinnitus get worse with migraine?
Tinnitus can be associated with multiple types of headache disorders. One headache type where tinnitus is sometimes seen is migraine. Some patients report that their tinnitus worsens only and consistently during migraine attacks.
When I press my neck my tinnitus stops?
The last maneuver of gentle neck pressure, which occludes the ipsilateral jugular vein, is particularly important. If the sound stops, it is almost certainly due to venous sinus stenosis or another venous sinus cause, such as dehiscent jugular plate or diverticulum.
Can tinnitus cause headaches and neck pain?
Tinnitus is often associated other symptoms such as neck pain, headache, depression, and difficulty with memory and concentration.
Can tinnitus make you feel unwell?
New symptoms, such as hearing loss, dizziness, loss of balance, numbness or weakness on one side of the face, or nausea or vomiting. Tinnitus starts to occur in just one ear.
Why do I feel pressure in my head?
The most common causes are headache, migraine, or infection. Most conditions that cause pressure in the head go away on their own or respond to over-the-counter pain medication. However, intense or persistent pressure in the head may indicate a severe underlying medical condition.
What are the symptoms of head pressure?
Symptoms
- Dull, aching head pain.
- Sensation of tightness or pressure across the forehead or on the sides and back of the head.
- Tenderness in the scalp, neck and shoulder muscles.
What is one of the earliest signs of increased intracranial pressure?
A: Early signs and symptoms include: changes in mental status, such as disorientation, restlessness, and mental confusion. purposeless movements. increased respiratory effort.
What were your first signs of a brain tumor?
Symptoms
- New onset or change in pattern of headaches.
- Headaches that gradually become more frequent and more severe.
- Unexplained nausea or vomiting.
- Vision problems, such as blurred vision, double vision or loss of peripheral vision.
- Gradual loss of sensation or movement in an arm or a leg.
- Difficulty with balance.
What is a vestibular migraine?
A vestibular migraine is a nervous system problem that causes repeated dizziness (or vertigo) in people who have a history of migraine symptoms. Unlike traditional migraines, you may not always have a headache. There are many names for this type of problem. Your doctor might also call it: Migraine-associated vertigo.
Can migraines cause Meniere’s disease?
While endolymphatic hydrops is still thought to be the cause of Meniere disease, this theory has been challenged and migraine has been implicated as a common etiology between vestibular migraine and Meniere disease.
What is silent migraine?
If you have a silent migraine, it means you get any of the typical migraine symptoms except for one: pain. Your doctor may suggest medications or devices that can treat the problem. You can also help yourself by avoiding your migraine triggers.
What does a neurologist do for vestibular migraine?
Medicines. Your neurologist may prescribe one or more medications that can help reduce vestibular migraine symptoms. Certain medications can help prevent migraines from occurring, while others can reduce a migraine that you are already experiencing.
What is the most common trigger of vestibular migraine?
The top 5 most common triggers for vestibular migraine are;
- Stress and anxiety.
- Poor sleep – both too little, and too much!
- Hunger and dehydration – missing meals and not taking enough water.
- Dietary triggers – many common foods, especially caffeine.
- Hormonal changes – i.e. menstruation, menopause and in teenagers.
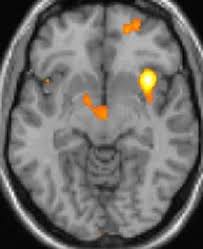
Can vestibular migraines be seen in MRI?
MRIs Find Abnormalities in Central Vestibular Cortex of Some Patients With Migraine. Magnetic resonance imaging (MRI) scans of patients with vestibular migraine reveal abnormalities in the central vestibular cortex, according to a study published in Brain and Behavior.
How do people live with vestibular migraines?
People with vestibular migraines can reduce the number and intensity of episodes by maintaining a regular sleep and meal schedule, avoiding triggers, exercising regularly and managing stress.
What is the best medication for vestibular migraine?
According to the available literature zolmitriptan 5 mg (tablet, nasal spray, and dissolvable tablet) should be the first choice in the acute vestibular migraine attack. Rizatriptan may also be used and analogous to migraine any other triptan may be just as effective (45).
What doctor treats vestibular migraines?
Vestibular migraines may be treated by an ENT (ear, nose, and throat) specialist, or otolaryngologist, and/or a neurologist.